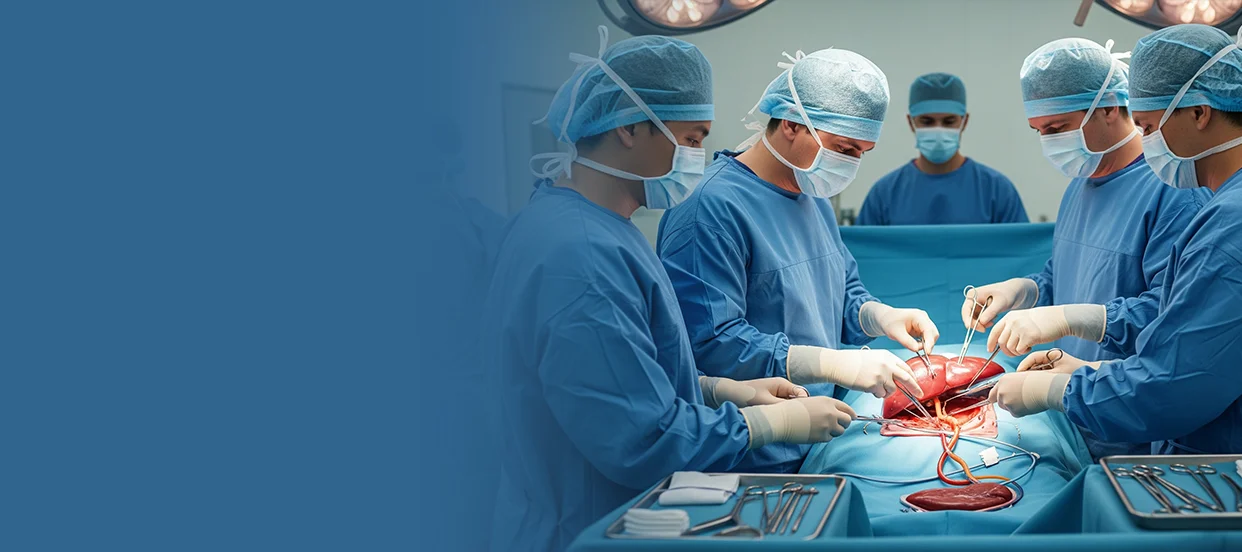
Liver transplantation is a life-saving procedure in patients with end-stage liver cancer, acute decompensated liver, or irreversible liver failure. This treatment includes the transfer of a normal liver from a cadaveric donor or a liver segment from a living donor to replace a malfunctioning liver. Due to the liver's regenerative ability, living-donor liver transplantation (LDLT) can be an enduring and rising method of treatment in India.
Your liver is the largest of the internal organs in your body and carries out essential functions of survival. It processes nutrients, drugs, and hormones; produces bile to digest fat; produces blood-clotting proteins; clears bacteria and toxins from the blood; and has an important role in immune function. If the liver ceases to function, these activities stop, leading to potentially fatal complications. This is why transplant surgery for the liver is often the only option when end-stage chronic liver disease or acute liver failure ensues.
Liver transplant is reserved for patients whose liver function is greatly impaired due to cirrhosis, chronic hepatitis, fatty liver disease, or genetic disorders like Wilson's disease. For acute liver failure due to drug poisoning or rare diseases, it can be life-saving. Surgery is the final choice when standard medical treatment has no value and must be performed in order to restore health and avoid death.
Unfortunately, the need for liver transplant exceeds the supply of available deceased-donor livers. In such a situation, a healthy individual can provide a portion of his or her liver. Since both donor and recipient liver regains its original size after transplantation, LDLT erases waiting lists and increases access to advanced liver transplantation.
Yes. Over the last decade, India has emerged as a leading destination globally for liver transplant surgery due to novel techniques, robust infrastructure, and exceptional outcomes. Advanced procedures such as laparoscopic donor hepatectomy, robotic assisted transplant, and computer-assisted perfusion systems are now common at best centers such as Medanta, Apollo, Fortis, Max, and Artemis. Sophisticated multidisciplinary teams would typically perform advanced transplants, with a combination of procedures such as cardiac or biliary repair, testifying to the advancement of India's transplant culture.
Patients understandably inquire about success rates, and the following are reassuring:
The pre-transplant evaluation is all-encompassing and tailor-made. Candidates undergo the following: MELD or PELD scoring, imaging, cardiovascular evaluation, and laboratory tests. Donors are evaluated for liver volume, blood group, metabolic status, and psychologic readiness. Nutritional and psychologic guidance, drug abuse service, and social work assessment are coordinated for the recipient and possible donor to ensure safe operation and convalescence.
When a donor live is found, surgery involves the removal of the diseased liver and the insertion of the healthy graft. The surgery lasts 6 to 12 hours, during which time blood vessels and bile ducts are carefully connected. Minimally invasive laparoscopic surgery commonly uses in living donor procurement, accelerating donor recovery. Advanced imaging, robotics assistance, and anesthesia monitoring improve outcomes by lessening risk and trauma.
Patients spend 2 to 3 weeks in the hospital with close intensive care monitoring to prevent things like infection, bile leak, or rejection. They are prescribed lifelong immunosuppressive drugs like tacrolimus to prevent rejection. Patients get out of bed and start eating quickly, and they get to go home when they stabilize and begin regaining their strength.
Post-discharge care involves strict medication adherence, dietary restrictions, and regular follow-up appointments for liver function tests, drug levels, and vital signs. In the long run, patients must live healthy, no alcohol, healthy eating, exercise regularly, and hepatitis and pneumococcus immunizations. With best care, the majority of liver transplant recipients live 20–30 years or more with excellent quality of life.
Recovery proceeds as below:
Liver transplant surgery in India would be around ?25–35 lakh (USD 30,000–45,000). Subsidized operations at certain government and charitable centers cost around ?12 lakh. Access is still boosted, however. Even with travel and accommodation expenses factored in, costs are substantially lower than in Western countries, yet without compromising quality or outcomes.
Yes, many international patients make the journey to India for world-class liver transplant centers. These patients must get medical visas, follow ethical protocols, and typically find suitable living donors. The majority of Indian centers provide full facilitation with visa arrangements, hospital booking, language translation, and post-operative care coordination.
While liver transplantation is highly successful, risks exist. Potential complications include organ rejection, infection due to immunosuppression, bile leaks, or vascular issues. Long-term medication side effects may include hypertension, high cholesterol, diabetes, or bone thinning. Nonetheless, regular medical follow-up and patient compliance reduce these risks significantly.
Despite impressive progress, India faces persistent issues:
India offers a compelling blend of surgical expertise, state-of-the-art technology, excellent outcomes, and international affordability for the process of liver transplantation. Whether in India or abroad, patients with liver failure can place their trust in Indian surgeons and hospitals with compassionate, up-to-date care. Appropriate planning, sound medical counsel, and follow-up over time render liver transplantation in India not just a therapy, but a second lease on life.